9 Min Read
What Every Senior Should Know About Psoriasis
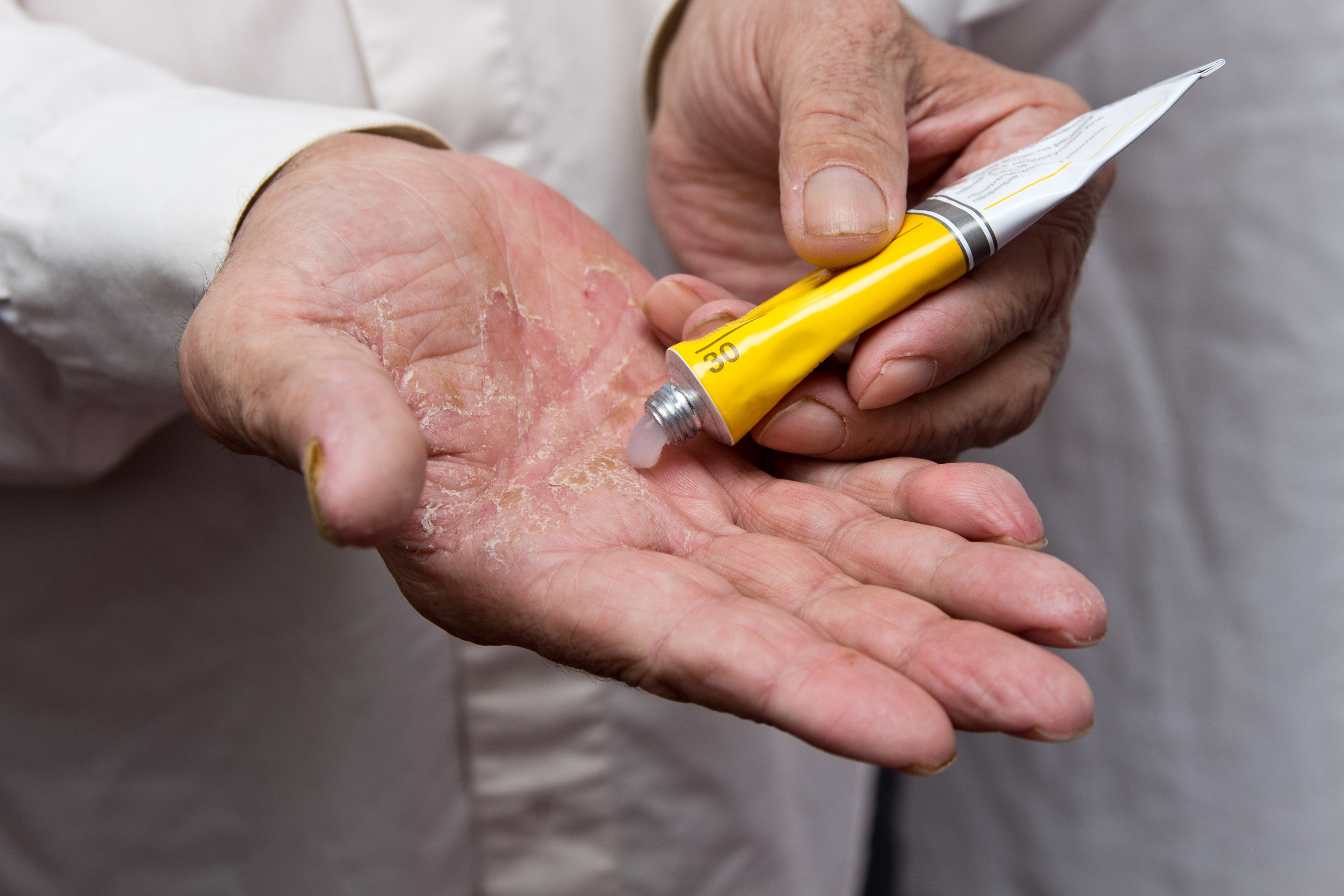
Psoriasis, a condition that causes the body to make new skin cells in days rather than weeks, causes thick, scaly patches that often appear on the knees, elbows, lower back, scalp, nails, and joints.
Symptoms tend to worsen with age, and psoriasis can be linked to other conditions that affect seniors, including type 2 diabetes, inflammatory bowel disease, and heart disease. Though not contagious, senior psoriasis is one of the more serious of skin diseases. It often progresses into a chronic condition, and there’s no known cure.
Causes of Psoriasis
Doctors are still unsure what causes an estimated 7.5 million Americans (or 2 percent of the U.S. population) to have psoriasis. Scientists have learned that genes and the immune system may play a role. When a person has psoriasis, for example, T-cells begin to attack the body’s skin cells, causing the body to make new cells more frequently. Once T-cells begin to attack, they continue attacking for the rest of the person’s life.
Scientists have also found that psoriasis runs in families. However, it’s not so cut and dry. Some people with psoriasis don’t have the genes that increase their risk of getting psoriasis, and others have the genes that increase their risk but never develop psoriasis.
Because of this, scientists believe that other factors also trigger psoriasis to appear for the first time. These include:
- Stress
- Skin injuries, like cuts or burns
- Infections
- Some medications, including prednisone, hydroxychloroquine, and lithium
- Weather, especially cold and dry
- Tobacco
- Alcohol
Psoriasis Signs in Seniors
There are eight different types of senior psoriasis that may develop, each with their own symptoms.
Plaque psoriasis—The most-common form accounts for about 80 to 90 percent of people with senior psoriasis. Symptoms include:
- Patches of thick, raised skin called plaques
- Scale (a dry, thin, and silvery-white coating) over some plaque
- Plaques of different sizes
- Smaller plaques joined together to form larger ones
Guttate psoriasis—This tends to appear after infection. Patches on the skin appear:
- Small and scaly
- Salmon to pink in color
- Temporary, often clearing in a few weeks or months without treatment
Inverse psoriasis—This often develops in areas where skin touches skin (armpits, genitals, etc.) Symptoms include:
- Smooth, red patches of skin that look raw
- Little, silvery-white coating
- Sore or painful
Pustular psoriasis—This type causes pus-filled bumps that usually appear on the feet and hands. Symptoms include:
- Red, swollen skin dotted with pus-filled bumps
- Extremely sore or painful
- Brown dots (and sometimes scale) after the pus-filled bumps dry
Pustular psoriasis (generalized)—This type is serious and life-threatening, causing pus-filled bumps to develop. Call your doctor immediately if these symptoms appear:
- Dry, red, and tender skin
- Pus-filled bumps covering most of the skin, often developing within hours (pools of pus leak onto the skin after the bumps break open)
- Smooth, glazed surface when dried skin peels off
- A new crop of bumps may appear in a few days or weeks
Erythrodermic psoriasis—Serious and life-threatening, this type of senior psoriasis needs immediate medical care. Symptoms include:
- Skin that appears burnt
- Chills, fever, and extremely ill appearance
- Muscle weakness, a rapid pulse, and severe itch
- Hypothermia may set in quickly, if unable to keep warm
Psoriasis in nails—About half of people with plaque psoriasis also see signs of psoriasis on their nails at some point. These include:
- Tiny dents in nails
- White, yellow, or brown discoloration
- Crumbling, rough nails
- Lifted or unattached nails
- Build-up of skin cells underneath nails
Psoriasis in joints—Some people with psoriasis, especially the elderly, may develop a type of arthritis called psoriatic arthritis. Symptoms include:
- Swollen or tender joints, especially in fingers and toes
- Heel pain
- Swelling on the back of legs, just above the heel
- Stiffness in the morning that fades during the day
Treatment for Psoriasis
If you think you may have senior psoriasis, contact your doctor immediately. The sooner your visit, the sooner you can start a treatment plan that meets your unique needs. While every senior may require different treatment, your doctor may recommend one or a combination of the following:
- Topical ointments soothe itchy skin but may be demanding among the elderly. Senior patients may need a nurse or loved one to help apply the topical ointment, especially in spots that are hard to reach. Because seniors’ skin is more prone to allergic reactions, practice caution when using topical medications—what works for one person may not work for everyone.
- Phototherapy/PUVA therapy, a conventional therapy for psoriasis, can be used among the elderly. With this treatment, lasers destroy blood vessels that feed the psoriasis sites, causing them to fade. However, proceed with caution. For some elderly patients who’ve experienced psoriasis for a long time, solar keratosis may develop. This type of therapy can aggravate the symptoms of solar keratosis, so it’s not recommended in these scenarios.
- Psoriasis medications pose potential complications for elderly patients as they’re often on more than one kind of medication. For any new medication, start with a low dosage of about 5 mg per week in case of side effects. Some conventional medicines, like retinoid, can trigger pruritus, and others like cyclosporine are not recommended for seniors because the side effects are too strong. Finding the right solution differs for each psoriasis sufferer. Some acne treatments, like salicylic acid, may also work, and steroid creams used for cystic acne may also reduce redness and swelling.

0 Comments